Submit a claim
Haven’t claimed for your treatment or service? Find out how you can claim online.
Before you start, read our claiming checklist
Extras claiming
Hospital claiming
How to claim
- nib App
- Online member account
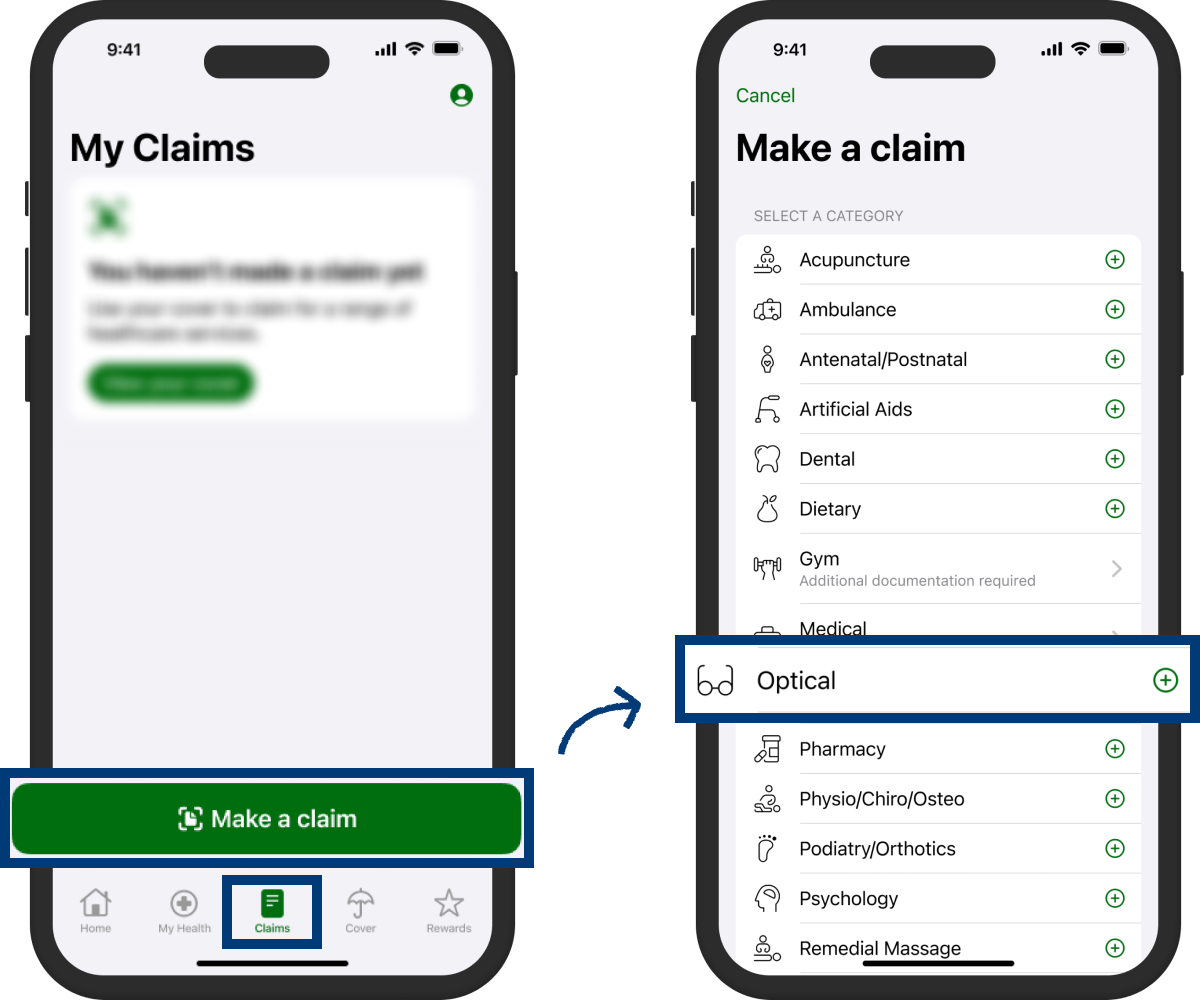
Select ‘Claims’ from the main navigation menu
Choose 'Make a claim'
Pick the category for the service you're claiming for. For example, if you are claiming glasses, select 'Optical'
For some categories, you might need to provide extra documentation. Once you select your category, we’ll tell you exactly what’s neededYou can either scan your receipt or upload a photo or document of it
Make sure your documents are clear and readable, as blurry images may lead to claim rejectionIf you are happy with your claim, select 'Submit claim'.